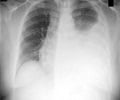
Antibody protection may help control infection with the bacteria that causes tuberculosis (TB), revealed scientists.

‘Antibody protection may help control infection with the bacteria that causes tuberculosis (TB), revealed scientists.’





In their study receiving online publication in Cell, the research team describes finding consistent differences in both the structure and function of antibodies targeting the TB bacteria between individuals with active TB disease and those with latent TB, which neither produces symptoms nor can be transmitted. The findings may lead to better ways of distinguishing between active and latent disease and to a more effective vaccine against tuberculosis.
"Ending tuberculosis by 2030 is one of the targets of the World Health Organization's newly adopted Sustainable Developmental Goals," says Lenette Lu of the Ragon Institute and the Massachusetts General Hospital (MGH) Department of Medicine, a co-lead author of the Cell report. "A more effective vaccine against TB could substantially contribute towards that goal, impacting the nearly one in three people worldwide who are infected and addressing the leading killer of individuals infected with HIV."
BCG is believed to work by stimulating cellular immunity, which is carried out by specialized immune cells including T cells and the macrophages that are directly infected by TB bacteria. Previous investigations into a possible role for antibodies in the immune response to TB have had conflicting results, but the Ragon team - led by Galit Alter, of MGH Department of Medicine and Sarah Fortune of the Harvard T.H. Chan School of Public Health - used a novel approach.
In addition to binding to their target pathogens and marking them for destruction by the immune system, antibodies also directly stimulate pathogen-killing cells of the innate immune system by binding to a cell-surface protein called the Fc receptor. The Ragon team profiled TB-specific antibodies from 22 individuals with latent TB and 20 with active TB for 70 different features associated with Fc-mediated antibody function. They first identified nine characteristics that differentiated between antibodies of the two groups of participants, and further investigation identified the biomarker that best distinguished between them.
Advertisement
Co-lead author Amy Chung now at the Peter Doherty Institute for Infection and Immunity in Melbourne, Australia - a joint venture between The University of Melbourne and The Royal Melbourne Hospital - explains, "This is a completely new area of immune research in tuberculosis, since these antibodies don't just recognize the infection, they also recruit immune cells to target it. People with latent infection have inactive disease for a reason, and if antibodies are playing a role in controlling the infection, the mechanism they use could be harnessed for future vaccine development."
Advertisement
"These findings - which could lead to major advances in the fight against one of humanity's oldest diseases - would have been impossible without visionary philanthropists like Terry and Susan Ragon, whose major gift created the Ragon Institute in 2009, and Mark and Lisa Schwartz, whose long-term support provided seed funding for Dr. Alter's work," says Peter Slavin, president of Massachusetts General Hospital, where the Ragon Institute is administratively based.
Source-Newswise