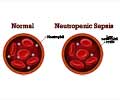
New test can determine whether antibiotics will be effective against certain bacterial infections (sepsis) and help physicians make faster and better prescription treatment choices.

‘New test developed for bacterial infections like sepsis results in better patient outcomes as it is a targeted antibiotic therapy.
’
Read More..




The results demonstrate that providing rapid, accurate drug susceptibility information to physicians could improve the care of patients with sepsis, a potentially life-threatening condition caused by the body’s response to an infection.Read More..
According to Ritu Banerjee, MD, Ph.D., associate professor of Pediatrics at Monroe Carell Jr. Children’s Hospital at Vanderbilt, time is of the essence.
"Patients are placed on a standard course of antibiotics when they initially present with possible sepsis," said Banerjee, the principal investigator of the RAPIDS-GN trial. "These antibiotics may be ineffective, or conversely, too broad-spectrum. Conventional culture and susceptibility testing methods take days for results to identify the bacteria and drug resistance. "Instead of waiting days for results, we can now get them in hours." Banerjee and her colleagues sought a way to shorten the wait time until the appropriate medication could be started to treat the infection.
RAPIDS-GN is the first multicenter, prospective, randomized controlled trial to compare the outcomes of patients with Gram-negative bloodstream infections who had blood culture testing with standard-of-caree culture and antibiotic susceptibility testing versus rapid organism identification and phenotype antibiotic susceptibility testing.
The study looked at the outcomes of 448 patients -- 226 received conventional care while 222 were randomized to the new testing method.
Advertisement
Conventional testing can take two to three days before the bacteria in the blood, and its drug resistance is fully identified. Utilizing the rapid testing method gave medical teams final results in about 12 hours.
Advertisement
"This was a very positive result. It was proof that faster actionable results led to timelier, targeted antibiotic therapy. The hope is that this, in turn, leads to better patient outcomes, less unnecessary broad-spectrum antibiotic use, and less emergence of drug-resistant organisms."
Banerjee also hopes the study results prompt more diagnostic companies to continue the development of platforms that will enable more rapid bacterial identification and resistance detection.
"One of the challenges is the cost of the testing because rapid testing methods are more expensive than conventional methods," she said. "The overarching goal is to improve outcomes for patients with sepsis."
Source-Eurekalert