Surgeons in Germany have found that making a small technical change to keyhole surgery for prostate cancer can reduce the occurrence of a common postoperative complication.
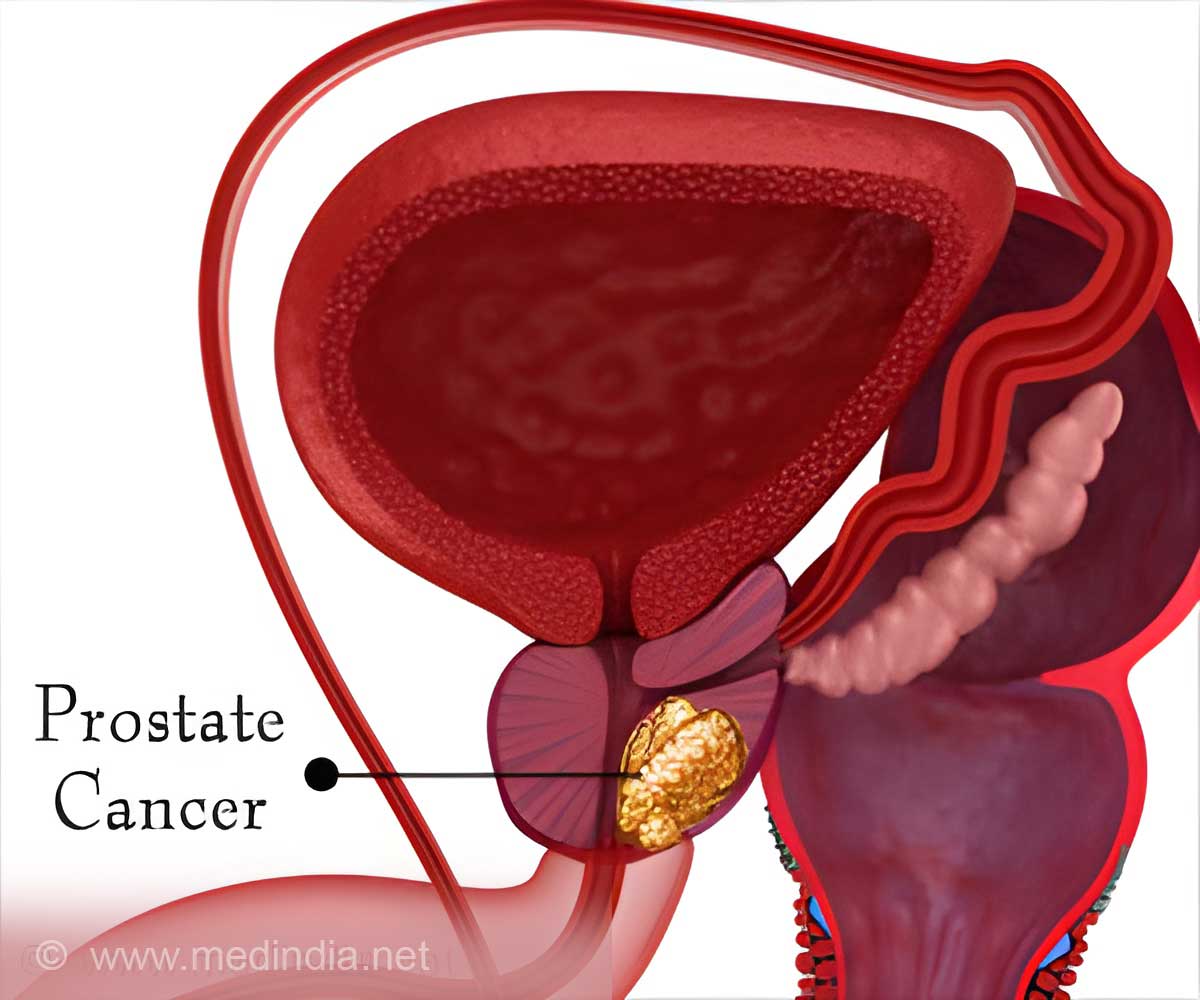
‘Keyhole surgery for prostate cancer can be significantly improved by a small technical adjustment, according to German surgeons, who found that this modification can reduce one of the most common post-operative complications.’





The findings are presented at the 2023 European Association of Urology annual Congress in Milan. Innovative Surgical Method Improves Outcomes for Prostate Cancer
Around 10 percent of patients whose prostate cancer and lymph nodes are removed through robot-assisted keyhole surgery require treatment for symptoms caused by lymphatic fluid collecting in the pelvis, known as lymphocele.Lymphocele can also be seen in nearly a third of patients when they were systematically checked, without them reporting symptoms.
Symptoms include superinfection, pain in the pelvis, pressure on the bladder, and swollen legs due to compression of the veins. If left untreated, symptomatic lymphocele can lead to serious infections or deep vein thrombosis.
Draining a lymphocele can take from three days to three weeks, with treatment complete only when the fluid is no longer accumulating. For some patients, this requires a stay in the hospital.
Advertisement
“Previous studies of the technique have been inconclusive, so we designed a larger, more robust trial to ensure our findings were statistically significant.”
Advertisement
New Technique Halves Risk of Lymphocele
The trial involved over 550 patients and four different surgeons working at University Medical Centre Mannheim, who were only informed whether a patient was to have a peritoneal flap once the rest of the operation had been completed.Patients were also randomized between the two groups – with a flap or without – taking into account other factors that might increase the risk of lymphocele, such as diabetes, the extent to which lymph nodes were removed, whether they took anti-coagulants and the surgeon doing the operation.
The patients were followed up for six months following the operation. During the six-month follow-up period, only 10 patients in the peritoneal flap group had developed a symptomatic lymphocele, compared to 25 in the control group.
At the time of discharge, 20 patients in the flap group had lymphocele with no symptoms, compared to 46 in the control group. During the follow-up, this had risen to just 27 in the flap group, but 74 in the control group.
Professor Philip Nuhn, Professor of Urology at University Medical Centre Mannheim, who led the research, said: “Using the peritoneal flap reduced the incidence of lymphocele from nine percent to less than four percent. We now use this as the new standard in Mannheim, and hope that – following these results – it will become common practice elsewhere as well.”
Professor Jochen Walz, from the EAU Scientific Congress Office and the Institut Paoli-Calmettes Cancer Center in Marseille said: “Most problems in these operations are linked to the lymph node removal, rather than the prostate surgery itself. Removal of the lymph nodes allows us to see if cancer has spread, so it’s important to do, particularly as surgery is now mainly used in higher-risk patients. Creating a peritoneal flap is a simple, small, easy, and quick procedure that takes about five minutes to complete. It is totally safe and this trial has shown it can substantially reduce complications, so there’s no reason why surgeons should not now do this as standard.
“Randomised control trials to evaluate technical changes in surgery are notoriously difficult to do – but this study has shown that they are both possible and effective. That’s good news for surgeons and for patients, who will benefit from better outcomes as a result.”
Source-Eurekalert





![Prostate Specific Antigen [PSA] Prostate Specific Antigen [PSA]](https://www.medindia.net/images/common/patientinfo/120_100/prostate-specific-antigen.jpg)